Calvin Underwood was born prematurely. The little boy required tube feeding throughout the first few weeks of his life. Ashley Simon was the nurse and education specialist at Cincinnati …
In March of 2016, Greenville, South Caroline police Officer Allen Jacobs was shot and killed on duty by a 17-year-old gunman. The fallen hero left behind his wife, Meghan. …
With three children, Dawn and Brad Bailey had no intention of ever adopting a foster child. Then, during Thanksgiving 2015, a local television station aired an episode of A …
We all sleep, but did you know that the way you sleep says a lot about who you are as an individual? For instance, Leonardo da Vinci took 20-minute …
How hard do you try to protect the environment? Are you aware of climate changes? Experts have created a few energy-saving strategies in order to reduce the effect of …
Steven Pladl, 42, of Knightdale, and his daughter Katie Pladl, 20, were arrested on incest charges after having a love child last year and reportedly getting married. Pladl has also …
An unidentified man was returning home from a hunting trip in Utah when Transportation Security Administration agents discovered a dead cougar in his luggage. According to Metropolitan Police Lt. David …
The family of a South Carolina woman who gouged her own eyeballs out in a drug-induced haze wants to warn others about the dangers of addiction. Kaylee Muthart, 20, …
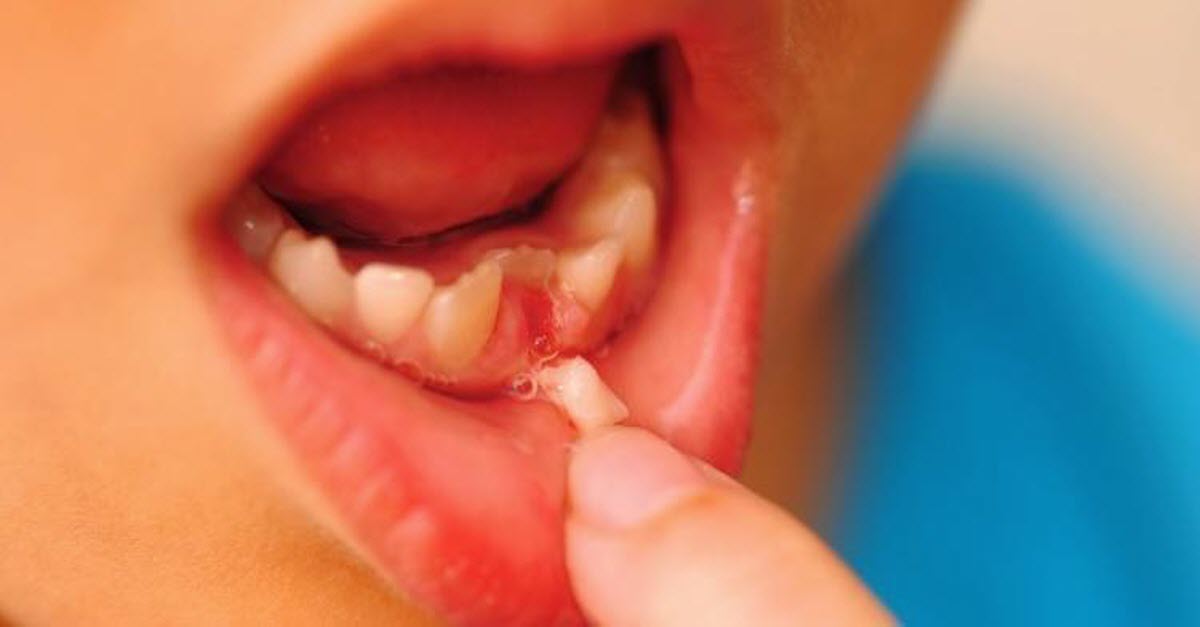
The next time your child has a loose tooth, you might want to tell the Tooth Fairy to sit this one out. Teeth contain stem cells in their dental …
What Lori and Chris Coble experienced is an insurmountable amount of pain. One fateful day, while Lori was driving her three children Kyle, Emma, and Katie home, disaster struck. …